HTF SF Healthcare Finance Recap (10/26/17)
This is a recap of the latest HTF SF Healthcare Finance event where three speakers shared their expertise with healthcare financing.
Susan Pantely is a principal and consulting actuary in the San Francisco office of Milliman. She provides actuarial and consulting services to a broad range of clients, including Blue Cross/Blue Shield plans, HMOs, commercial insurers, government agencies, and healthcare providers. Her work includes rate development, provider contract review, reserve certification, capitation development, Medicare risk feasibility studies, HMO start-ups, HMO due diligence, and development of risk sharing and reimbursement arrangements for physician groups, PHOs, ACOs, and other integrated delivery systems. In addition, Susan has extensive experience with the valuation, financial analysis, and projection of healthcare services for several state public health insurance (Medicaid) programs.
An Unchanging System
Susan begins her talk by joking that not much has changed from her presentation in 20 years.
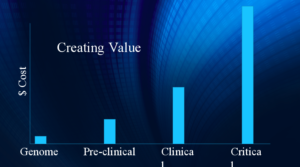
Much of the information in her slide deck has stayed the same, because the healthcare system has stayed the same. Though we are starting to focus on getting value out of our healthcare costs, we’ve not hit a tipping point where the value-based model trumps the volume-based model. The U.S. has the highest cost of healthcare per capita in the world, but cost is not an issue if we are receiving quality. We are not getting nearly enough value for our dollars.
Our healthcare system is fragmented, resulting in no coordination of care, and we end up with high levels of variation in utilization patterns across country that can’t just be explained by patient demographics. In other words, there’s a lot of waste and inefficiencies in our system that aren’t justifiable.
Quality and Outcomes
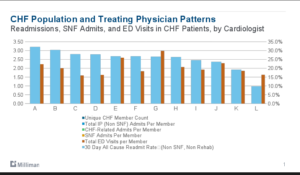
As a country, we’re moving toward a value-based system with a focus on quality and outcomes. Milliman is helping this transition by looking at quality metrics by provider such as how many of their patients are going to the ED and what that doctor may be doing or not doing to contribute to this.
Example of some provider metrics Milliman looks at.
Doctors want to spend time with patients and not have to think about the financial incentives. So Milliman establishes utilization targets that are reasonable for each organization, and provides medical management to help achieve those targets. Rationalizing care is superior to rationing it, and the focus on delivering the best care at the right time for the right patient will help control utilization and costs.
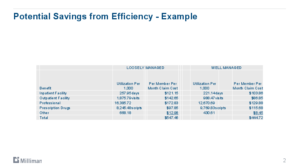 Savings from efficiency is one of things preached by Susan’s firm. Unfortunately haven’t seen a whole lot of movement in last 10-15 years. In CA, delivering the right care at the right time can save around $100 of healthcare costs per person, per month.
Savings from efficiency is one of things preached by Susan’s firm. Unfortunately haven’t seen a whole lot of movement in last 10-15 years. In CA, delivering the right care at the right time can save around $100 of healthcare costs per person, per month.
Providers are beginning to take on more financial risk and having payments tied to outcomes. But because many consumers prefer freedom of choice for healthcare, when they choose to go out of network for their care, it causes attribution problems. It’s hard to measure and pay for value when the patient is receiving care from various sources.
In an article Susan wrote called “Whose patient is it?”, she examines the different factors that contribute to a patient’s health outcome and the difficulty in attributing complete health outcome ownership.
Payment Mechanisms
- Bundle payments for an episode of care where surgery, and doctor and readmissions are included provide incentives for providers to prevent readmissions. This works well for services that have low variation like a hip replacement. But for something like asthma or cancer, it’s difficult to bundle together.
- CMS is trying to do cancer bundle payments, but one fixed fee for an episode of cancer seems ambitious because there are many different cancer types and variations.
- Pay for performance: giving physicians bonuses based on performance. Varying degrees of risk. Providers may lose payment, and dynamic system of patients moving in and out of population makes it difficult to measure performance. Demographics shift during the year, and catastrophic incidents have to be adjusted for. New drugs and new technologies that come out during the year also can’t be priced into options. Not easy arrangements because of the different dynamics going on.
Predictive Modeling
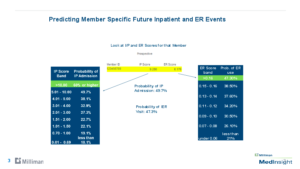
Example of predictive modeling.
- Assigning patient risk scores in population health analytics to assess for probability of admission
- 20 years ago a lot of providers lost money on these deals. Now there’s better tools to monitor population (which patients at risk, what we can do to prevent critical care)
- Long term improvements. Takes time, since claims take awhile to get paid and outcomes are not short-term results. Initiatives take awhile to measure so long-term thinking is needed
Consumer Role
There are many moving parts in the healthcare system, and a value-based model doesn’t do a complete job of accounting for all the dynamic factors. CMS penalizes for readmissions, but sometimes that can’t be controlled by the provider. The patient’s behavior has an influence in care outcomes and individual decisions and the role of the consumer must be taken into consideration for a comprehensive value-based payment model.
Uli Chettipally, MD., MPH, is a physician, researcher, and innovator at Kaiser Permanente. He is a speaker on topics bridging artificial intelligence and clinical practice that can improve the quality, cost, and convenience of care. He is the co-founder and Chief Technology Officer of CREST Network, a multi-center, collaborative network that encourages, enables, and executes research in emergency medicine. CREST Network covers 21 hospitals with a total of 1.2 million emergency patient visits per year in Northern California. His other roles include a) President, Society of Physician Entrepreneurs, San Francisco Bay Area chapter b) Editor and Member of the Board of Directors, San Mateo County Medical Association c) Assistant Clinical Professor of Medicine, University of California, San Francisco.
Two Models of Healthcare
Uli draws the analogy between volume and value-based care by telling the story of two college students who come from different financial backgrounds.
One student has a parent who pays for everything from tuition to living expenses, while the other student must work different jobs to pay for college. Both go to same school and take the same classes. But one has access to an abundance of resources while the other must focus on where to dedicate their energy and focus to achieve their goal of graduating. The outcome will be roughly the same for both students when they end up with college degrees, but how they get there is the difference between volume and value-based care models.
- Volume-based care: you can have anything you want (student with parental support)
- Value-based Care: figure out how to spend your limited resources (student who must work)
High Cost, Low Quality Care
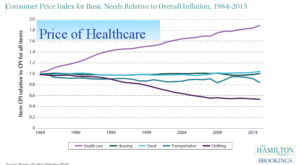
The rising cost of healthcare outpaces inflation.
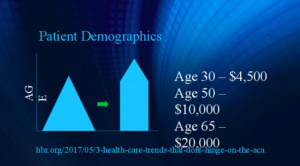
The cost of healthcare care depends heavily on age, and the aging U.S. population is growing rapidly. If the current system doesn’t change, healthcare costs will rise even higher:
Cost of healthcare compared to age.
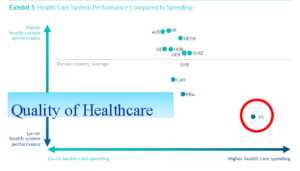
Despite high costs, the U.S. has a low quality of care compared to other countries:
- Uli says that 50% of what we do in a typical U.S. clinical practice is unnecessary, ineffective or dangerous. His research tries to find out which services are wasteful by pulling data from EHRs and using descriptive analytics. The goal is to predict what will happen to patients based on historical data and come up with prescriptive analytics to recommend a path for physicians and patients to follow to improve outcomes and control costs.
- Uli views heart attacks as failures of the healthcare system. Kaiser members enjoy a 30 – 50 % lower chance of having a heart attack or stroke due to upstream prevention. When Uli first started with Kaiser, there was 1 – 2 heart attacks each week in the ER. The last time he saw a heart attack in the ER was 3 months ago. The rates of heart attacks have dropped due to prevention initiative and controlling risk factors.
- Past: Surgery. We operated on everything from ulcers to tonsils.
- Present: Medication used to treat most diseases now.
- Future: Moving toward diet and behavioral interventions. Holistic approach.
Costs by care segments.
Going upstream to manage exercise, medication, sleep, diet, will control costs. That is why Kaiser is seeing such a sharp decline in strokes and heart attacks. They are aggressive on controlling risk factors and this translates to lower downstream costs. The future will be controlling genome with precision and personalized medicine.
Health is an Information business
We need to figure out how to accumulate and analyze data, assess risk, and implement actionable data-driven strategies. The sooner we can figure out how to do this effectively and at scale, the sooner we will be able to control healthcare costs.
Peggy Bui, MD, MBA is a physician leader at CareMore Health, a subsidiary of Anthem, which delivers integrated care and health coverage to Medicare and Medicaid patients. At CareMore, Peggy focuses on quality improvement projects to optimize post-discharge follow-up, patient outcomes, and preventative health for high-risk populations. Peggy also serves as a part-time Clinical Instructor in the Division of Hospital Medicine at the UCSF. She joins CareMore after completing residency training in Internal Medicine at the University of California – San Francisco, where she was a key member of several system-wide initiatives as a part of the Health, Society and Leadership area of distinction. During residency, she also spearheaded the creation of an EMR-based clinical decision tool to guide more cost-effective use of high cost heart failure medications. She has an interest in bringing technology-driven innovations to healthcare and has collaborated on low-cost medical applications and devices such as ValveStrong and EarTrumpet. She previously worked as a consultant at Monitor Deloitte, advising Fortune 500 companies on corporate strategy, government affairs, finance, and marketing. She also advised several medical startups while completing her dual MD/MBA degree from UC Irvine.
History of CareMore Health
- CareMore Health is an integrated care delivery model serving Medicare/Medicaid populations that focuses on chronic care management. The founder of CareMore wanted to focus on the sickest of the sick and manage care more properly. CareMore started as a health plan funded by the founder and his physician friends. It launched in the early 90s, but operated at a loss in the first few years because the organization devoted much resources to keeping patients healthy (an early value-based care model) during a time when the compensation wasn’t rewarding value based care.
- Restructured as a Medicare Advantage plan in the late 90s and moved over to a capitated plan that received a lump sum of payments to keep patient population healthy. Within 3 years they were profitable and had exponential YOY membership growth.
- In 2011, CareMore acquired by Wellpoint (now Anthem for $800million).
Concierge Medicine and Upstream Value
Caremore expanded after the acquisition and its goal is to reach 1 million members in all 50 states. CareMore is a health plan and care delivery model, and is considered to be concierge Medicine for the chronically ill. This means the doctor goes where the patient goes. For example, they would admit the patient to hospital, and if the patient is transferred to ICU, the doctor will go there with them. This ensures a continuity of care and that there’s a provider who understands the needs of the patient.
CareMore’s mantra is to intervene upstream and prevent downstream.
The company profits through outcomes, and the difference in its model is the amount of time devoted to patients. They employ more staff to patients than any other company in the industry. This is based on core belief that every dollar spent saves multiple dollars in the future. As a result, member costs are 20% lower than industry averages.
Patient Focus
- CareMore focus on patients with multiple co-morbidities and medical issues.
- Patients who enroll with CareMore can keep their PCP since there’s many that CareMore contracts with and they even reach out to PCPs who patients want to keep their PCPs (granted their health outcomes are acceptable with CareMore’s standard).
- When patients join the plan, patients get triaged into special programs (renal disease, diabetes, heart diseases, etc) and patients classified as higher risk have a team formed around them (case manager, social worker, mental health, etc.). The team follows the patient and even visits the patient at home. High-touch care points early on to prevent them going to ED.
- In our fragmented healthcare system – a chronically ill patient will see an average of 11 doctors without any care coordination. Typically only an overworked PCP and a few specialists to prevent this patient from being critically ill. CareMore has dedicated care centers that serve as chronic care management centers with care coordinators and case managers who are reviewing and monitoring population health data to look for red flags.
- The outcomes speak for themselves: CareMore patients have a 40% lower admission rate compared to traditional Medicare and 19% shorter length of stay. This is fueled by the capitation plan (incentivized to keep patients healthy) which motivates providers to look for different ways to keep patient healthy and out of the hospital.
Benefits and Needs
CareMore syncs benefits with needs. For example, many patients don’t drive anymore and don’t have rides to and from appointments. CareMore sends Lyft rides to take patients home, to the gym and to the clinic as a part of their benefits. Members always get a Lyft ride for a post-discharge visit to a doctor regardless of the plan they have. There are also various health and fitness classes to engage elderly folks to keep active.
Valued-Based Payment Model
- CareMore has value-based care baked into its model. Their providers are all paid based on performance, and receive a competitive base salary and quarterly bonus based on quality metrics along with stock options also based on quality metrics (i.e. hospital admission rates, 30-day readmission rates, patient LOS, whether records were reviewed when patients left hospital, BMI, appropriate diabetes care, kidney function, fall risk, medication adherence, colonoscopies, mental health assessments in last 12 months, et.). These metrics are how everyone from sales to IT are paid and everyone has a stake in keeping patient healthy.
- PCPs aren’t hired. CareMore contracts with PCPs at a cost-sharing program that incentives them to keep patients healthy. Only contracts with nursing facilities with 5-star CMS ratings. Quality is a focus on every aspect of the operation, from how employees are paid to which facilities, PCPs and specialists are contracted with. CareMore doesn’t own hospitals, they can go to whatever hospital and caremore doctor will go see them.
- CareMore’s innovative service model will likely be seen more in the future because the financial incentives are aligned with value-based care and married to outcomes.
- When there are the same directional incentives for all stakeholders, that is when there will be reduced friction and efficiency in healthcare.
When providers get a set budget or amount of money to take care of a population of patients, they be more motivated to keep the population healthy. This belief is at the care of CareMore’s model, and as we move ahead we will likely see more care delivery models that are similar to CareMore.